Palmitoylethanolamide (PEA) is a natural compound that your body produces in response to various forms of cellular damage. Its primary role is to promote homeostasis, which is the body’s ability to maintain a stable and balanced internal environment for optimal functioning and overall wellness. (1)
It can also be found in certain foods. In fact, PEA was originally identified in the 1950s as an active anti-inflammatory agent in egg yolk. This discovery was made after researchers observed that children who consumed a diet rich in eggs seemed to be protected against rheumatic fever. (2)
Potential Health Benefits of PEA
Since its discovery, PEA has been the subject of extensive research due to its ability to target multiple pathways in the body to restore cellular health. This versatility grants PEA a wide range of health benefits, particularly in terms of its anti-inflammatory, pain-relieving, and neuroprotective effects.
“Therefore, dietary supplementation of PEA and congeners substantially overcomes the classical pharmacology view of “one drug, one target, one disease”, opening a whole new era in the management of animals’ health, i.e., an according-to-nature biomodulation of body responses to different stimuli and injury.” (2)
Congeners of PEA are compounds derived from the same starting molecule and are similar in structure and function.
Pain
The therapeutic potential of PEA for pain relief has been an exciting research focus because it targets both pain and inflammation simultaneously. By modulating the body’s inflammatory response and reducing pain sensitivity, PEA offers a potential solution for individuals suffering from chronic pain and inflammation-related conditions.
The efficacy and safety of PEA has been shown in numerous clinical trials investigating its use for conditions marked by pain, including joint pain, neuropathic pain, post-operative pain, headaches, and endometriosis (1).
A recent systematic review and meta-analysis evaluated PEA in the treatment of chronic pain. Eleven studies, describing a total of 774 patients, were analyzed.
The researchers found that PEA significantly increased functional ability and improved the quality of life in individuals suffering with chronic pain. Additionally, they found that PEA treatment is not associated with any side effects.
“The results of this systematic review and meta-analysis suggest that PEA is an effective and well-tolerated treatment for chronic pain.”
Joint Pain
A study evaluated the efficacy of PEA for relieving symptoms of knee osteoarthritis. Participants were divided into groups to receive daily doses of 300 mg PEA, 600 mg PEA or placebo for 8 weeks.
They found PEA significantly lowered pain and stiffness, with pain decreasing by 40% (300 mg group) and by 49.5% (600 mg group). Notably, anxiety levels were significantly lower in the PEA groups.
PEA also showed superior pain relief compared to ibuprofen in a trial for temporomandibular joint (TMJ) osteoarthritis. Pain intensity ratings decreased progressively, and after 7 days, the PEA group had a significantly greater decrease in pain compared to the ibuprofen group.
Low Back Pain
Low back pain (LBP) is considered chronic when the pain is present for three months or longer. It is commonly associated with anxiety and panic disorders, depression, and sleep trouble.
A pilot study evaluated PEA as add-on therapy to Tapentadol (TP), a pain reliever, for 6 months in chronic low back pain (LBP) management.
Pain intensity was measured using the visual analog scale (VAS).
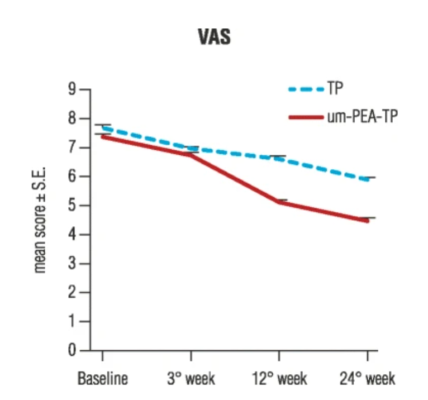
The figure illustrates pain intensity scores over 24 weeks for two groups: TP alone (dashed blue line) and TP with PEA (solid red line)
Results showed that PEA supplementation for 24 weeks significantly reduced pain intensity scores compared to TP alone. PEA also reduced the level of disability and the dosage of TP required to manage pain.
The benefits of PEA observed in this study have been reinforced in numerous clinical trials on conditions marked by chronic LBP, including failed back surgery syndrome and sciatica pain.
Headache
Headaches involve a complex interplay of nerve dysfunction, activation of pain pathways, inflammation in blood vessels, and heightened sensitivity to pain.

PEA is recognized for its anti-inflammatory and pain-relieving properties, making it an intriguing candidate for addressing these underlying mechanisms and providing relief for headache sufferers.
In a study involving individuals with tension-type headaches, PEA was found to be as effective as ibuprofen in reducing headache severity and duration. Remarkably, it demonstrated greater efficacy in resolving severe headaches.
Similarly, in a pilot study on adults with migraines already taking NSAIDS, PEA administration resulted in a significant reduction in migraine pain, which lasted throughout the study period.
Nonsteroidal anti-inflammatory drugs (NSAIDs) are over-the-counter medications commonly used to reduce inflammation and pain.
Gastrointestinal Tract
The gut microbiota plays a crucial role in nutrient metabolism, immune function, and gut barrier integrity, and is essential for maintaining a healthy gut.
Dysbiosis, which is a shift in the composition of bacteria in your gut, is closely associated with chronic diseases.
A recent review emphasized the significance of gut dysbiosis in autoimmune diseases.
“This review suggests that the altered gut bacteria in patients with autoimmune diseases may be closely related to abnormal immune activity and weakened anti-inflammatory activity.”
In a study using mice with compromised gut health, PEA administration increased the levels of beneficial bacteria and reduced inflammation in the gut. They found that PEA improved the barrier that protects the intestine and stimulated the growth of new cells in the colon.
“In this respect, PEA has been referred to as an intestinal “gate keeper”, whose increased levels contribute to locking of the gut barrier and to the reduction of intestinal inflammation.” (2)
In a clinical trial, a combination of PEA and polydatin improved abdominal pain in patients with irritable bowel syndrome (IBS).
Polydatin is a dietary compound found in grapes that has antioxidant and anti-inflammatory activity.
Furthermore, it has been shown that PEA has a positive impact on colitis, a form of inflammatory bowel disease (IBD).
Several investigations in mouse models of colitis reported that PEA reduced the production of inflammatory molecules, inhibited the movement of immune cells from circulation into the colon, and lowered overall inflammation. (3,4)
Brain Health
Research suggests that PEA is produced “on demand” during inflammatory and neurodegenerative conditions to protect against inflammation and neuronal damage. (5)
“Among these naturally occurring molecules, palmitoylethanolamide (PEA) has been independently associated with neuroprotective and anti-inflammatory properties, raising interest into the possibility that its supplementation might represent a novel therapeutic approach in supporting the body-own regulation of many pathophysiological processes potentially contributing to neurocognitive disorders.” (6)
“Body-own regulation” refers to the natural ability of our bodies to regulate and control various processes internally. The author is saying that PEA supplementation is like a boost or support to the body’s innate ability to take care of itself and maintain optimal functioning.

Neurodegeneration
While neurodegenerative diseases encompass a range of conditions, they share common characteristics. These conditions involve progressive damage to specific areas of the brain responsible for movement, muscle coordination, mood, and cognition.
In patients with Parkinson’s Disease (PD), the addition of PEA to the standard treatment regime led to a significant and progressive reduction in both motor and non-motor symptoms of PD. The study also found a decrease in the number of patients experiencing symptoms after one year of PEA treatment. (10)
Additionally, a study in patients with Multiple Sclerosis (MS) found that supplementation of PEA (600 mg) reduced injection site pain from standard therapy and significantly improved quality of life. PEA also progressively decreased levels of inflammatory molecules in the blood over the 12 month trial period (depicted in the figure below). (11)
This figure represents the serum levels of IFN-ɣ, one of the inflammatory molecules measured in this study, in the placebo group (white bars) and the PEA group (black bars).
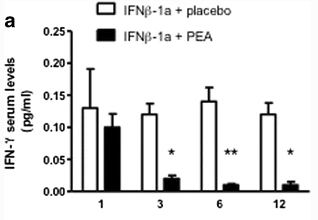
Initially, on the left, no significant difference was observed between the groups. However, from months 3 to 12, the PEA group consistently showed significantly lower IFN-ɣ levels.
Depression
PEA interacts with key brain systems involved in mood regulation and stress responses, showcasing its potential as an antidepressant agent.

A clinical trial involving individuals with major depressive disorder (MDD), found that the addition of PEA as an add-on therapy to a common antidepressant medication resulted in improved depressive symptoms, with noticeable improvements observed as early as week 2.
Numerous preclinical studies have indicated that PEA may possess antidepressant properties, as observed in cases where depression is associated with conditions like neuropathic pain, traumatic brain injury, and neurodegeneration.
However, more extensive research is required to establish and understand the specific anti-depressant effects of PEA.
Traumatic Brain Injury
- In a mouse model of mild TBI, PEA alleviated psychiatric dysfunctions and improved behaviors related to pain, emotions, and recklessness. (12)
- In another animal study, PEA reduced brain swelling, regulated inflammation, and prevented cell death.
- Treatment with PEA after brain injury limited damage, reduced tissue loss, and enhanced recovery in mice. (13)
Conclusion
PEA offers diverse health benefits by harnessing the body’s own system to promote cellular health. Its unique ability to target pain and inflammation provides a comprehensive approach to pain management, gut health, and neuroprotection.
Importantly, PEA demonstrates a remarkable safety profile with minimal side effects, which is particularly valuable when considering its application to conditions of pain and inflammation.
References
- Palmitoylethanolamide: A Natural Compound for Health Management
- Palmitoylethanolamide and Related ALIAmides: Prohomeostatic Lipid Compounds for Animal Health and Wellbeing
- Palmitoylethanolamide improves colon inflammation through an enteric glia/toll like receptor 4-dependent PPAR-α activation
- Palmitoylethanolamide, a naturally occurring lipid, is an orally effective intestinal anti-inflammatory agent
- Palmitoylethanolamide (PEA) as a Potential Therapeutic Agent in Alzheimer’s Disease
- Therapeutic effect of palmitoylethanolamide in cognitive decline: A systematic review and preliminary meta-analysis of preclinical and clinical evidence
- Palmitoylethanolamide Protects Against the Amyloid-β25-35-Induced Learning and Memory Impairment in Mice, an Experimental Model of Alzheimer Disease
- Palmitoylethanolamide Dampens Reactive Astrogliosis and Improves Neuronal Trophic Support in a Triple Transgenic Model of Alzheimer’s Disease: In Vitro and In Vivo Evidence
- Neuroprotection by Association of Palmitoylethanolamide with Luteolin in Experimental Alzheimer’s Disease Models: The Control of Neuroinflammation
- Ultra-micronized Palmitoylethanolamide: An Efficacious Adjuvant Therapy for Parkinson’s Disease
- Oral Palmitoylethanolamide Treatment Is Associated with Reduced Cutaneous Adverse Effects of Interferon-β1a and Circulating Proinflammatory Cytokines in Relapsing–Remitting Multiple Sclerosis
- Palmitoylethanolamide Reduces Neuropsychiatric Behaviors by Restoring Cortical Electrophysiological Activity in a Mouse Model of Mild Traumatic Brain Injury
- N-Palmitoylethanolamine-Oxazoline as a New Therapeutic Strategy to Control Neuroinflammation: Neuroprotective Effects in Experimental Models of Spinal Cord and Brain Injury

